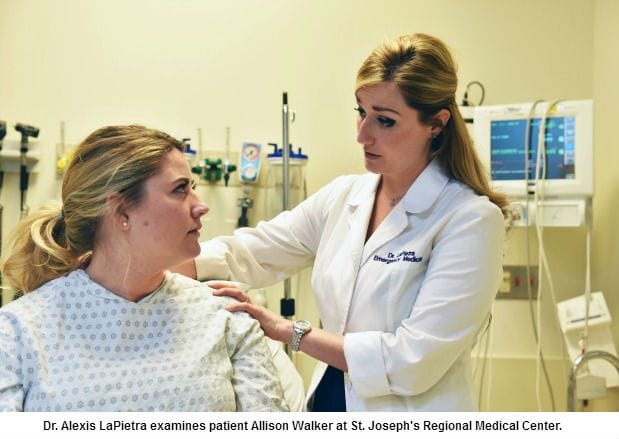
By now, bringing up the opioid epidemic in America is like talking about the weather—everyone knows about it but no one can control it. As the Medical Director of Pain Management in the Emergency Department at St. Joseph’s Regional Medical Center, Dr. Alexis LaPietra knows this conversation a bit too well. Having dealt with pain often at its most visceral level, she understands how she, as a physician, is innately pulled into the problem. From tending to patients suffering from acute pain to chronic pain, she had to take a step back at one point and consider how she was contributing. She says, “I kept seeing the spectrum [of pain] and wondered if we’re somewhat responsible for some of the people who are prescribing opiates moving onto addiction and possibly, ultimately, death.”
That question didn’t just sit there for long. In January 2016, St. Joseph’s launched ALTO (Alternatives to Opiates Program), the first program in the nation curbing the use of opiates in the ER, spearheaded by LaPietra herself. Using targeted non-opioid medications, trigger point injections, nitrous oxide and ultrasound guided nerve blocks, the goal is to attack what LaPietra calls “the frontline of pain” with alternatives rather than what has become almost a traditional prescription for 30 pills of Oxycodone. In addition to alternative medicine, the program also embraces a variety of holistic modalities (from harp music to pranic healing to acupuncture) in conjunction to their overall treatment.
Despite all the innovative remedies being used at St. Joseph’s, one of the largest focuses of the ALTO program still remains to be basic education. “We educate the patients right up front when they have acute pain and talk about alternatives,” LaPietra says. “We try to involve the patient in the decision-making, empower them to appreciate the full-spectrum of medications available, so that their past experience doesn’t have to continue to dictate their future care.” This means that even if opiate medications like oxycodone or hydrocodone may have been effective for many patients in the past, it may not be the best route for them to go today under this program. As Dr. LaPietra iterates to everyone who comes under her care, “The more exposure you have to opiates, the higher your risk is to dependency.”
Understandably so, things may be a bit more complicated for chronic pain patients. For these individuals, the staff does allow the issuance of opiates, but only to a point. “We do try to avoid refilling opiate prescriptions for patients who have established care with somebody,” Dr. LaPietra explains. “So if a patient comes in with chronic pain that has flared up, and is causing them an acute issue, we will manage their pain in the emergency department. But, if they’ve run out of the oxycodone that they’ve been getting for years from Dr. Smith, we’re not going to refill that because we feel as that’s irresponsible.” Patients who are dependent or do have issues with opiate addictions may not be happy with that, but physicians nevertheless take the opportunity to plant the seed and at least have an important discussion about addiction.
However, even with the ongoing conversations taking place between the medical personnel and patient, the greatest piece of the puzzle may actually be educating the general public about pain: what it is and why it’s sometimes important. “If you look internationally, we consume the most opiates,” LaPietra says. “However, I know from watching the news that we are certainly not a nation that has the most pain in the world.” So it’s important to ask ourselves, why are we consuming all the opiates? In LaPietra’s perspective, it could be a cultural dynamic. “More than saying ‘I have zero pain’ or ‘I have ten pain,’ I think we need to talk about a patient's tolerable or intolerable pain, and let them know that the reality of pain management in 2016 is that we will probably be able to take away the majority of someone’s pain, but to say you’re going to be pain-free is unrealistic and not attainable.”
It’s easy to see how a single physician may not think that he or she is contributing much to the opiate overdose epidemic, but after speaking with LaPietra, it’s evident that fighting the epidemic needs to be an effort in everyone’s part. There’s no “one recipe” that will solve it all and each patient with pain should be treated on a case-by-case level. Yes, it’s a little bit more work on the physician’s level, but LaPietra presents a dire scenario as reminder: “If we continue at this rate, then tens of thousands of young people are going to continue to die—and that is just not an acceptable side effect because we want to just give something strong.”
While small changes are happening all over the nation, the ALTO program has taken an enormous leap in creating a successful, system-wide approach. With that, comes a lot of responsibility. Looking forward, LaPietra has her eyes set on continuing to strengthen her program in the ER, where there are 55 attending physicians, 24 residents and 180 nurses and “to be very transparent about what we’ve done so that it can be replicated everywhere.” As the opiate epidemic affects everyone in the house of medicine, the end goal for LaPietra and everyone involved is “to have [ALTO] be something that can be adopted as a national model in whatever way that is applicable for each institution and that, as a unified front nationally, we can decrease patient exposure to opiates.” Decreasing patient exposure to opiates inevitably decreases the addiction potential, which then also decreases the number of overdose deaths—and if you ask me, that’s hitting the opiate epidemic right where it hurts.
If you or someone you know is seeking help from opiate addiction, please visit our directory of opiate and detox treatment centers or call 866-606-0182 to start the path to recovery today.